Last Updated on December 25, 2022
Introduction / Definition
Pathological jaundice | Physiological jaundice | Prolonged jaundice
Definition
• Pathological jaundice occurs within 24 hours of life
• Prolonged jaundice: visible jaundice (or serum bilirubin >85 µmol/L) that persists beyond 14 days in life in term infant or 21 days in preterm infant
Implications
• Unconjugated bilirubin → deposited in basal ganglia → kernicterus
Risk Stratification – Low Risk, Medium Risk, High Risk
Risk stratification
1st rule: Gestational age
2nd rule: Risk factors
– Isoimmune haemolytic disease (mother blood group O+ve / mother Rhesus negative)
– G6PD deficiency
– Neonatal encephalopathy
– Neonatal asphyxia
– Sepsis
| 35 – 376/7 weeks | ≥38 weeks | |
| Low risk | — | No risk factor |
| Medium risk | No risk factor | With risk factors |
| High risk | With risk factors | — |
NOTE: Presence of >1 risk factor will NOT further increase the risk!! Examples:
– 38 weeks + G6PD deficiency = Medium risk
– 38 weeks + G6PD deficiency + Mother O+ve = Medium risk (not high risk)
=====
Re-stratification of risk
Upgrading: from low to medium risk // from medium to high risk
Downgrading: from high to medium risk // from medium to low risk
Example:
37 weeks + Mother O+ve = high risk
Later on results of baby’s ABO is O+ve, direct Coombs test negative
Re-stratified into medium risk
Investigations
Neonatal jaundice surveillance
• Transcutaneous bilirubinometry (TCB)
Neonatal jaundice workup
• Total serum bilirubin (TSB)
• Full blood picture or Full blood count
• Reticulocytes
• Patient’s ABO + RhD
• Patient’s direct Coombs test
• Trace mother’s blood group
**Not all NNJ require ABO & Coombs test, unless suspicious of ABO incompatibility
Other investigations
• G6PD
• Blood C&S, urine C&S if infection/sepsis suspected
Neonatal jaundice (inpatient) monitoring
• TCB or TSB
Treatment Options
1. Phototherapy
• ‘Intensive phototherapy’ = ‘double phototherapy’
=====
2. Exchange transfusion
ET guideline for babies ≥35 weeks gestation
• Indications of ET:
–> Signs of acute bilirubin encephalopathy (ABE), or
–> TSB >85 µmol/L above ET level
–> TSB rises to ET levels despite intensive phototherapy
3. IV Immunoglobulin (IVIG)
Phototherapy Level & Exchange Transfusion Level
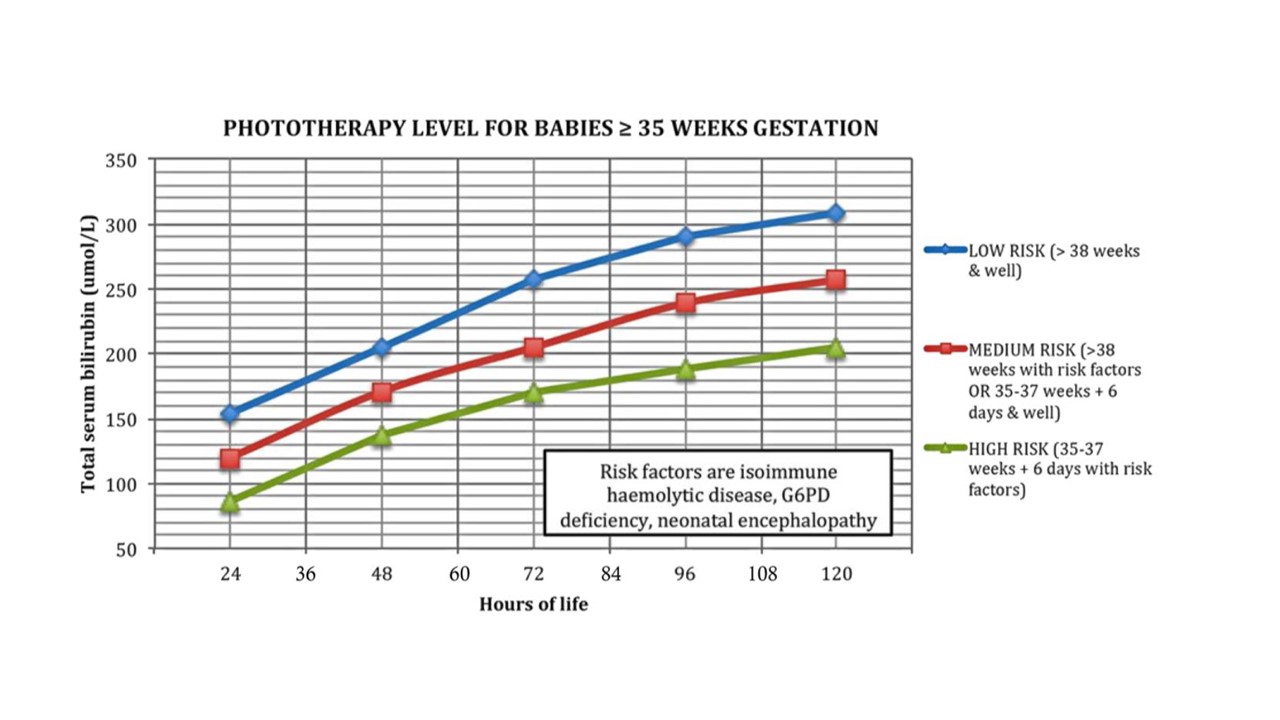
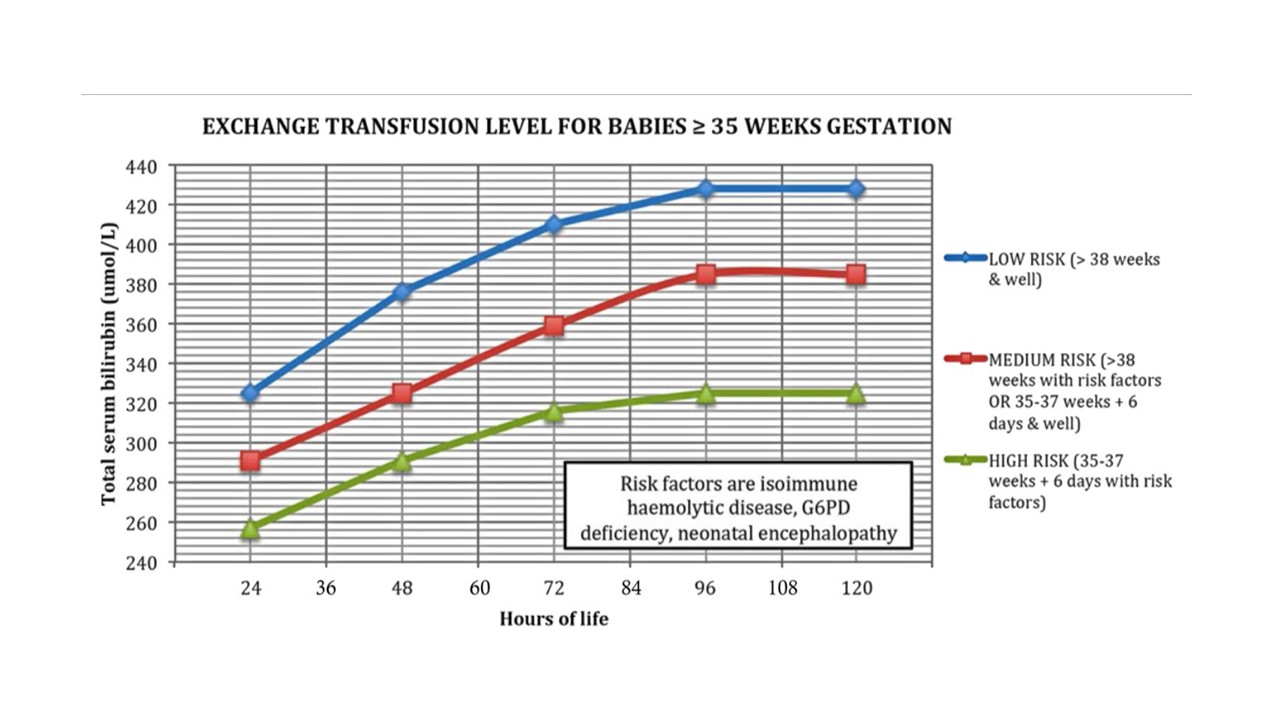
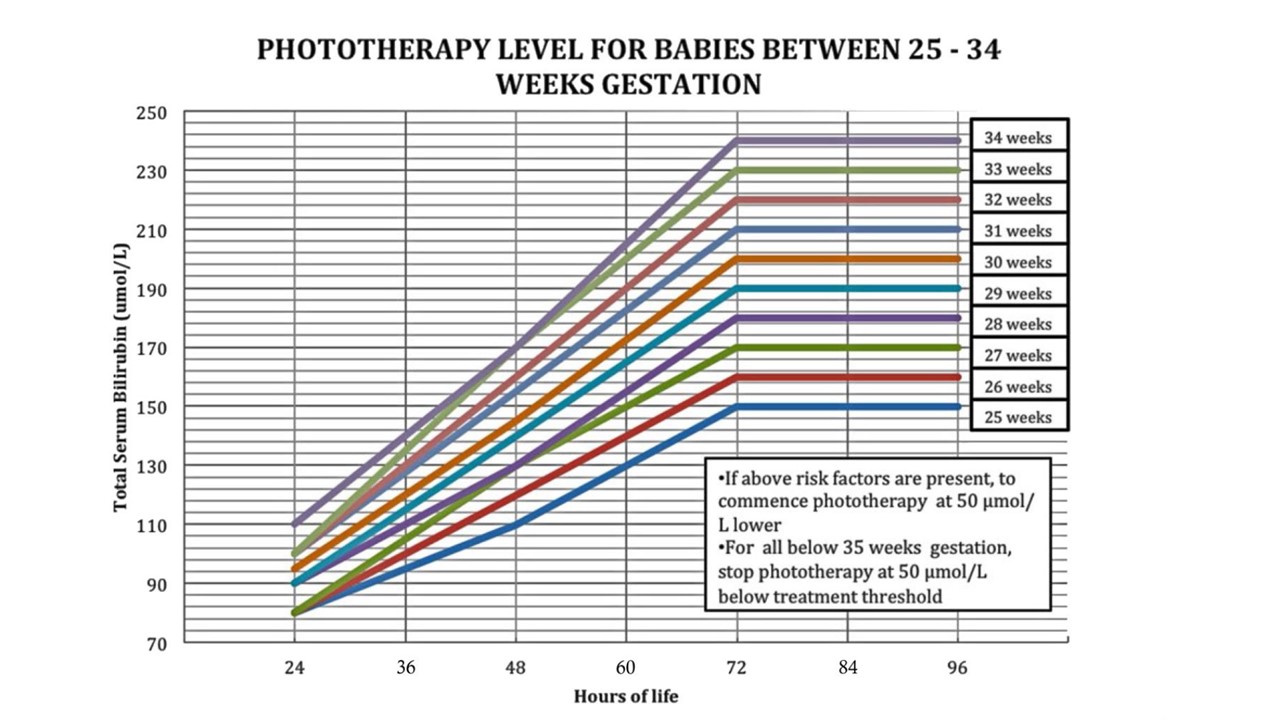
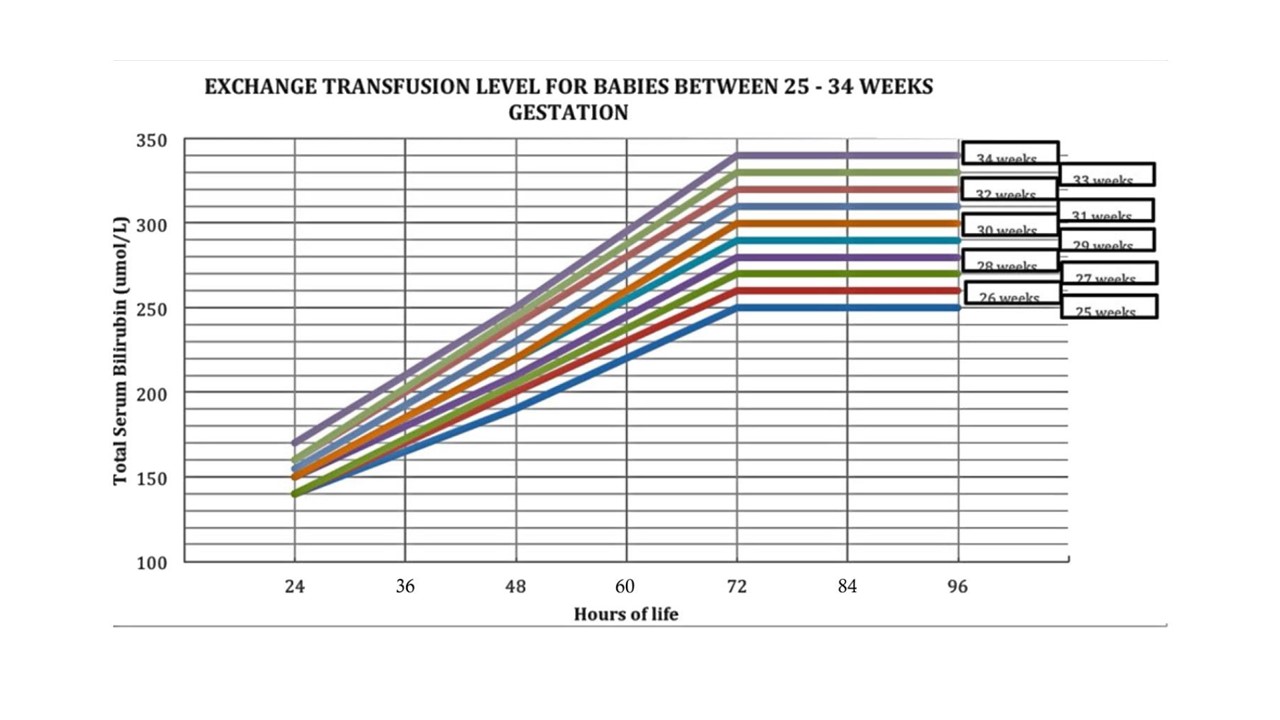
Prolonged jaundice
Causes
(i) Conjugated hyperbilirubinaemia (>25 µmol/L)
• Biliary tree abnormalities e.g. biliary atresia
• Neonatal hepatitis
• Metabolic disorders e.g. alpha-1 antitrypsin deficiency, citrin deficiency
(ii) Unconjugated hyperbilirubinaemia
• Haemolytic anaemia e.g. G6PD deficiency, congenital spherocytosis
• Hypothyroidism
• Infection, e.g. UTI, TORCHES
• High GI obstruction e.g. pyloric stenosis
Signs & symptoms e.g.
• Pale stool
• Poor weight gain
• Pallor
• Hepatosplenomegaly
Prolonged jaundice workup
• Total serum bilirubin (+direct & indirect)
• FBC + reticulocytes // FBP
• Liver function test
• Thyroid function test
• UFEME ± Urine C&S
• Trace G6PD screening taken at birth
—– —– —– —– —–
Other Ix
• TORCHES
• HBsAg, Anti-HCV
• Alpha I antitrypsin
Imaging
• USG HBS
Take Home Messages
1. Physiological jaundice is a diagnosis of exclusion
2. Whenever there is a NNJ, the underlying cause should be sought and documented in case note
3. It’s important to stratify the risks correctly to prevent missed phototherapy
4. When TCB is higher than photo level, you can document the plan to start phototherapy, and don’t forget to inform the nurse
5. TCB of more than 200 μmol/L is not reliable, and requires TSB stat to confirm the bilirubin level, but you can still start phototherapy if TCB higher than photo-level
References
1. Paediatric protocol (4th ed)